From the new 2010 resuscitation guidelines:
For attempted defibrillation of children 1 to 8 years of age with an AED, the rescuer should use a pediatric dose-attenuator system if one is available. If the rescuer provides CPR to a child in cardiac arrest and does not have an AED with a pediatric dose-attenuator system, the rescuer should use a standard AED. For infants (<1 year of age), a manual defibrillator is preferred. If a manual defibrillator is not available, an AED with pediatric dose attenuation is desirable. If neither is available, an AED without a dose attenuator may be used.

Summary: Adult AEDs may be used in all infants and children if there is no child-specific alternative
Highlights of the 2010 American Heart Association Guidelines for CPR and ECC
Tag Archives: APLS
Resuscitation Guideline Changes
New CPR Guidelines
The International Liaison Committee on Resuscitation has published its five-yearly update of resuscitation guidelines.
The American Heart Association Guidelines can be accessed here
The European Resuscitation Guidelines can be accessed here
2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science
Circulation. 2010;122:S639
Weight formula for kids
The traditional ‘APLS formula’ for weight estimation in children based on age (wt in kg = [age+4] x 2) is recognised as underestimating weight in ‘developed’ countries, with the degree of underestimation increasing with increasing age.
Several authors have attempted to derive a more accurate formula.
In the UK, the measured weights of over 93 000 children aged 1-16 who attended a paediatric emergency department were used to compare a previously derived formula (wt=3[age]+7) with the APLS formula.
The formula ‘Weight=2(age+4)’ underestimated children’s weights by a mean of 33.4% (95% CI 33.2% to 33.6%) over the age range 1–16 years whereas the formula ‘Weight=3(age)+7’ provided a mean underestimate of 6.9% (95% CI 6.8% to 7.1%); this latter formula remained applicable from 1 to 13 years inclusive.
The authors state: ‘The APLS formula has clearly become a victim of better nourished children. With a mean underestimate of more than 20% (nearly 40% at age 10 years), its place as a weight estimation tool is questionable…. To continue with an inaccurate formula with no evidence base cannot be considered good medical practice.’
Weight estimation in paediatrics: a comparison of the APLS formula and the formula ‘Weight=3(age)+7’
Emerg Med J. 2010 Jul 20. [Epub ahead of print]
A previous retrospective Australian study on over 70 000 paediatric ED attendances derived formulae for three different age ranges:
- For Infants < 12 months: Weight (kg) = (age in months + 9)/2
- For Children aged 1-5 years: Weight (kg) = 2 x (age in years + 5)
- For Children aged 5-14 years: Weight (kg) = 4 x age in years.
Make your Best Guess: An updated method for paediatric weight estimation in emergencies
Emerg Med Australas. 2007 Dec;19(6):528-34
Terlipressin for refractory cardiac arrest in kids
Okay so it’s a small case series – but the results warrant further investigation: 10-20 mcg/kg terlipressin was given to five infants and children who arrested in the paediatric intensive care unit and who had not responded to several doses of adrenaline (epinephrine)1. Sustained return of spontaneous circulation (ROSC) was achieved in four, and two survived to be discharged home without sequelae and with good neurologic status at 6 and 12 month follow up. Interestingly, the four patients who had ROSC all had septic shock as the cause of their arrest. The two survivors had severe bradycardia and severe bradycarda-asystole as the arrest rhythms, and both received 20 mcg/kg terlipressin.
Terlipressin is a synthetic arginine vasopressin analog with a significantly longer duration of effect, which previously showed positive effects when administered to a small group of children unresponsive to prolonged resuscitative efforts2.
1. Pediatric cardiac arrest refractory to advanced life support: Is there a role for terlipressin?
Pediatr Crit Care Med. 2010 Jan;11(1):139-41
2. Beneficial effects of terlipressin in prolonged pediatric cardiopulmonary resuscitation: A case series.
Crit Care Med. 2007 Apr;35(4):1161-4
Vital signs of severely injured children
Systolic blood pressures of severely injured children are very often hypertensive compared with APLS ‘norms’. A lower pulse rate is associated with more severe brain injury

Comparing the systolic blood pressure (SBP) and pulse rate (PR) in injured children with and without traumatic brain injury
Resuscitation. 2010 Apr;81(4):418-21
Kids need 'proper' CPR if non-cardiac cause of arrest
The American Heart Association recommends cardiopulmonary resuscitation (CPR) by bystanders with chest compression only for adults who have cardiac arrests, but not for children. These recommendations have new support in a large observational study from Japan examining outcomes in 5170 out-of hospital paediatric arrests over a 3 year period.
For children who had out-of-hospital cardiac arrests from non-cardiac causes, conventional CPR (with rescue breathing) by bystander was associated with improved outcomes compared with compression-only CPR (7·2% [45/624] favourable one month neurological outcome vs 1·6% [6/380]; OR 5·54, 2·52–16·99). In children who had arrests of cardiac causes conventional and compression-only CPR were similarly effective. Infants < 1 year had uniformly poor outcomes.
An editorial points out that this is the largest study that has analysed out-of-hospital cardiac arrest in children, and the overall survival of 9% with only 3% of children having a good neurological outcome, is consistent with previous reports.
Conventional and chest-compression-only cardiopulmonary resuscitation by bystanders for children who have out-of-hospital cardiac arrests: a prospective, nationwide, population-based cohort study
Lancet. 2010 Apr 17 345:1347-54
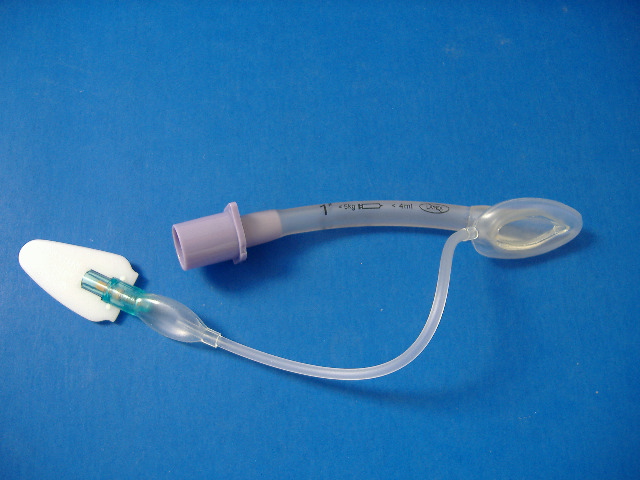
LMA for newborn resuscitation
An observational study of near term infants (34 weeks gestation to 36 weeks and 6 days) born in an Italian centre over a 5 year period showed that nearly 10% of near-term infants needed positive pressure ventilation at birth, confirming that this group of patients is more vulnerable than term infants. Most were able to be managed with either bag-mask ventilation (BMV) or with a size 1 laryngeal mask airway (LMA). Of the 86 infants requiring PPV, 36 (41.8%) were managed by LMA, 34 (39.5%) by BMV and 16 (18.6%) by tracheal intubation. Why not slap a tiny LMA on your neonatal resuscitation cart – it could come in handy!
Delivery room resuscitation of near-term infants: role of the laryngeal mask airway
Resuscitation. 2010 Mar;81(3):327-30
Paraldehyde in Paediatric Status Epilepticus
Data were collected on 53 episodes of paraldehyde use in tonic-clonic status epilepticus, which showed it appeared to be effective at terminating seizures in 33 of 53 cases. The median dose was 0.79 ml/kg, in keeping with current APLS guidelines (0.4 ml/kg of paraldehyde plus 0.4 ml/kg olive oil given per rectum)
Review of the efficacy of rectal paraldehyde in the management of acute and prolonged tonic-clonic convulsions
Arch Dis Child. 2009 Sep;94(9):720-3
Neonatal Emergencies
‘THE MISFITS’ is a popular mnemonic to assist in identifying the cause of critical illness in the neonatal period.
T = Trauma (Accidental and Non Accidental)
H = Heart Disease, Hypovolemia, Hypoxia
E = Endocrine (Congenital Adrenal Hyperplasia, Thyrotoxicosis)
M = Metabolic (Electrolyte Imbalance)
I = Inborn Errors of Metabolism
S = Sepsis (Meningitis, Pneumonia, UTI)
F = Formula Mishaps (Under or Over dilution)
I = Intestinal Catastrophes (Intussusception, Volvulus, Necrotizing Enterocolitis)
T = Toxins / Poisons
S = Seizures
From: Tonia J. Brousseau, Ghazala Q. Sharieff Neonatal Emergencies
http://cme.medscape.com/viewarticle/557824 accessed 29/12/09