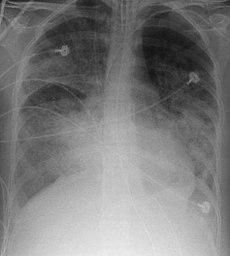
Here’s a heads up on a major evidence-based medicine event in critical care: the results of two long awaited randomised controlled trials assessing high-frequency oscillation (HFOV) in Acute Respiratory Distress Syndrome (ARDS) have both been published, and the full text is available from the New England Journal of Medicine at the links below.
In summary, the Oscillation for Acute Respiratory Distress Syndrome Treated Early (OSCILLATE)(1) and the Oscillation in ARDS (OSCAR)(2) trials showed no improvement in in-hospital death or 30 day mortality, respectively. OSCILLATE was terminated early on the basis of a strong signal for increased mortality with HFOV.
An editorial discusses some of the reasons why these outcomes were seen, which include among other factors the possibility that they were related to increased requirements for sedation, paralysis, and vasoactive drugs in the HFOV patients that were not offset by improvements in oxygenation and lung recruitment.
1. High-Frequency Oscillation in Early Acute Respiratory Distress Syndrome
NEJM 22 Jan 2013
[EXPAND Click for abstract]
BACKGROUND Previous trials suggesting that high-frequency oscillatory ventilation (HFOV) reduced mortality among adults with the acute respiratory distress syndrome (ARDS) were limited by the use of outdated comparator ventilation strategies and small sample sizes
METHODS In a multicenter, randomized, controlled trial conducted at 39 intensive care units in five countries, we randomly assigned adults with new-onset, moderate-to-severe ARDS to HFOV targeting lung recruitment or to a control ventilation strategy targeting lung recruitment with the use of low tidal volumes and high positive end-expiratory pressure. The primary outcome was the rate of in-hospital death from any cause.
RESULTS On the recommendation of the data monitoring committee, we stopped the trial after 548 of a planned 1200 patients had undergone randomization. The two study groups were well matched at baseline. The HFOV group underwent HFOV for a median of 3 days (interquartile range, 2 to 8); in addition, 34 of 273 patients (12%) in the control group received HFOV for refractory hypoxemia. In-hospital mortality was 47% in the HFOV group, as compared with 35% in the control group (relative risk of death with HFOV, 1.33; 95% confidence interval, 1.09 to 1.64; P=0.005). This finding was independent of baseline abnormalities in oxygenation or respiratory compliance. Patients in the HFOV group received higher doses of midazolam than did patients in the control group (199 mg per day [interquartile range, 100 to 382] vs. 141 mg per day [interquartile range, 68 to 240], P<0.001), and more patients in the HFOV group than in the control group received neuromuscular blockers (83% vs. 68%, P<0.001). In addition, more patients in the HFOV group received vasoactive drugs (91% vs. 84%, P=0.01) and received them for a longer period than did patients in the control group (5 days vs. 3 days, P=0.01).
CONCLUSIONS In adults with moderate-to-severe ARDS, early application of HFOV, as compared with a ventilation strategy of low tidal volume and high positive end-expiratory pressure, does not reduce, and may increase, in-hospital mortality. (Funded by the Canadian Institutes of Health Research; Current Controlled Trials numbers, ISRCTN42992782 and ISRCTN87124254, and ClinicalTrials.gov numbers, NCT00474656 and NCT01506401.)
[/EXPAND]
2. High-Frequency Oscillation for Acute Respiratory Distress Syndrome
NEJM 22 Jan 2013
[EXPAND Click for abstract]
BACKGROUND Patients with the acute respiratory distress syndrome (ARDS) require mechanical ventilation to maintain arterial oxygenation, but this treatment may produce secondary lung injury. High-frequency oscillatory ventilation (HFOV) may reduce this secondary damage.
METHODS In a multicenter study, we randomly assigned adults requiring mechanical ventilation for ARDS to undergo either HFOV with a Novalung R100 ventilator (Metran) or usual ventilatory care. All the patients had a ratio of the partial pressure of arterial oxygen (PaO2) to the fraction of inspired oxygen (FiO2) of 200 mm Hg (26.7 kPa) or less and an expected duration of ventilation of at least 2 days. The primary outcome was all-cause mortality 30 days after randomization
RESULTS There was no significant between-group difference in the primary outcome, which occurred in 166 of 398 patients (41.7%) in the HFOV group and 163 of 397 patients (41.1%) in the conventional-ventilation group (P=0.85 by the chi-square test). After adjustment for study center, sex, score on the Acute Physiology and Chronic Health Evaluation (APACHE) II, and the initial PaO2:FiO2 ratio, the odds ratio for survival in the conventional-ventilation group was 1.03 (95% confidence interval, 0.75 to 1.40; P=0.87 by logistic regression).
CONCLUSIONS The use of HFOV had no significant effect on 30-day mortality in patients undergoing mechanical ventilation for ARDS. (Funded by the National Institute for Health Research Health Technology Assessment Programme; OSCAR Current Controlled Trials number, ISRCTN10416500.
[/EXPAND]
![]() A letter in Intensive Care Medicine by Hoeper and colleagues from Hannover describes a small case series of six ARDS patients with severe hypoxaemia who went straight from non-invasive ventilation to awake veno-venous ECMO. All had single organ failure and four were immunocompromised, the latter factor influencing the decision to try to avoid invasive mechanical ventilation. Four of the six patients survived to hospital discharge. A larger multicentre study is being planned.
A letter in Intensive Care Medicine by Hoeper and colleagues from Hannover describes a small case series of six ARDS patients with severe hypoxaemia who went straight from non-invasive ventilation to awake veno-venous ECMO. All had single organ failure and four were immunocompromised, the latter factor influencing the decision to try to avoid invasive mechanical ventilation. Four of the six patients survived to hospital discharge. A larger multicentre study is being planned.