Body temperature raises heart rate and respiratory rate in kids, potentially affecting our interpretation of these clinical signs.
Dutch investigators developed centile charts of respiratory rates for specific body temperatures (derivation study), so that abnormally high rates could be identified as a means of predicting lower respiratory infection (validation set).
Respiratory rate increased overall by 2.2 breaths/min per 1°C rise (standard error 0.2) after accounting for age and temperature in the model, which is similar to a previous UK study that suggested a rise in respiratory rate of around 0.5-2 breaths per minute and an increase in heart rate of about 10 beats per minute for every 1 degree celcius above normal.
Cut-off values at the 97th centile were more useful in detecting the presence of LRTI than existing (Advanced Paediatric Life Support) respiratory rate thresholds.
The respiratory rate charts are available here.
Derivation and validation of age and temperature specific reference values and centile charts to predict lower respiratory tract infection in children with fever: prospective observational study
BMJ. 2012 Jul 3;345:e4224
Free Full Text Link
Tag Archives: paediatric
Lifting the Fogg on ED Intubaton
Fellow retrieval specialist and Royal North Shore Hospital emergency physician Dr Toby Fogg and coauthors have published their audit of intubations in an Australian Emergency Department(1). More important than the results themselves is that the process of monitoring ones practice inevitably leads to improvements. For example, at Toby’s institution an intubation checklist has been introduced since the audit began. Other Australasian EDs are encouraged to participate using the free resources at airwayregistry.org.au.
Recently we have also seen the publication of Korean registry data on paediatric intubations performed in 13 academic EDs over 5 years(2), in which first pass success rates (overall 67.6%) were higher with emergency physicians compared with paediatricians. Interestingly, a rapid sequence intubation technique was only used in 22.4% of intubations, which was more likely to be used by emergency physicians and was associated with a greater likelihood of first pass success.
This relatively low first pass success rate is reminiscent of the American study published in September(3) which raised some eyebrows with its 52% first pass intubation success rates in a paediatric ED, and which also showed that attending-level providers were 10 times more likely to be successful on the first attempt than all trainees combined. Possible reasons for such a low first pass success rate compared with adult registry data include the rigorous video analysis method used, or perhaps more likely that paediatric emergency subspecialists are exposed to fewer critical procedures, resuscitations, and intubations than their general emergency medicine counterparts(4).
As a specialty we must continue to seek to do better, and I salute all these brave authors who are telling it like it is. Particularly with children, whose airways are relatively easy, we have to develop the training, preparation, supervision, monitoring and feedback to aim for as high a success rate as possible.
1. Prospective observational study of the practice of endotracheal intubation in the emergency department of a tertiary hospital in Sydney, Australia
Emerg Med Australas. 2012 Dec;24(6):617-24
[EXPAND Click to read abstract]
OBJECTIVE: To describe the practice of endotracheal intubation in the ED of a tertiary hospital in Australia, with particular emphasis on the indication, staff seniority, technique, number of attempts required and the rate of complications.
METHODS: A prospective observational study.
RESULTS: Two hundred and ninety-five intubations occurred in 18 months. Trauma was the indication for intubation in 30.5% (95% CI 25.3-36.0) and medical conditions in 69.5% (95% CI 64.0-74.5). Emergency physicians were team leaders in 69.5% (95% CI 64.0-74.5), whereas ED registrars or senior Resident Medical Officers made the first attempt at intubation in 88.1% (95% CI 83.9-91.3). Difficult laryngoscopy occurred in 24.0% (95% CI 19.5-29.3) of first attempts, whereas first pass success occurred in 83.4% (95% CI 78.7-87.2). A difficult intubation occurred in 3.4% (95% CI 1.9-6.1) and all patients were intubated orally in five or less attempts. A bougie was used in 30.9% (95% CI 25.8-36.5) of first attempts, whereas a stylet in 37.5% (95% CI 32.1-43.3). Complications occurred in 29.0% (95% CI 23.5-34.1) of the patients, with desaturation the commonest in 15.7% (95% CI 11.9-20.5). Cardiac arrest occurred in 2.2% (95% CI 0.9-4.4) after intubation. No surgical airways were undertaken.
CONCLUSION: Although the majority of results are comparable with overseas data, the rates of difficult laryngoscopy and desaturation are higher than previously reported. We feel that this data has highlighted the need for practice improvement within our department and we would encourage all those who undertake emergent airway management to audit their own practice of this high-risk procedure.
[/EXPAND]
2. The factors associated with successful paediatric endotracheal intubation on the first attempt in emergency departments: a 13-emergency-department registry study
Resuscitation. 2012 Nov;83(11):1363-8
[EXPAND Click to read abstract]
BACKGROUND: We investigated which factors are associated with successful paediatric endotracheal intubation (ETI) on the first attempt in emergency department (EDs) from multicentre emergency airway registry data.
METHODS: We created a multicentre registry of intubations at 13 EDs and performed surveillance over 5 years. Each intubator filled out a data form after an intubation. We defined “paediatric patients” as patients younger than 10 years of age. We assessed the specialty and level of training of intubator, the method, the equipment, and the associated adverse events. We analysed the intubation success rates on the first attempt (first-pass success, FPS) based on these variables.
RESULTS: A total of 430 ETIs were performed on 281 children seen in the ED. The overall FPS rate was 67.6%, but emergency medicine (EM) physicians showed a significantly greater success rate of 74.4%. In the logistic regression analysis, the intubator’s specialty was the only independent predictive factor for paediatric FPS. In the subgroup analysis, the EM physicians used the rapid sequence intubation/intubation (RSI) method and Macintosh laryngoscope more frequently than physicians of other specialties. ETI-related adverse events occurred in 21 (7.2%) out of the 281 cases. The most common adverse event in the FPS group was mainstem bronchus intubation, and vomiting was the most common event in the non-FPS group. The incidence of adverse events was lower in the FPS group than in the non-FPS group, but this difference was not statistically significant.
CONCLUSIONS: The intubator’s specialty was the major factor associated with FPS in emergency department paediatric ETI, The overall ETI FPS rate among paediatric patients was 67.6%, but the EM physicians had a FPS rate of 74.4%. A well structured airway skill training program, and more actively using the RSI method are important and this could explain this differences.
[/EXPAND]
3.Rapid sequence intubation for pediatric emergency patients: higher frequency of failed attempts and adverse effects found by video review.
Ann Emerg Med. 2012 Sep;60(3):251-9
[EXPAND Click to read abstract]
STUDY OBJECTIVE: Using video review, we seek to determine the frequencies of first-attempt success and adverse effects during rapid sequence intubation (RSI) in a large, tertiary care, pediatric emergency department (ED).
METHODS: We conducted a retrospective study of children undergoing RSI in the ED of a pediatric institution. Data were collected from preexisting video and written records of care provided. The primary outcome was successful tracheal intubation on the first attempt at laryngoscopy. The secondary outcome was the occurrence of any adverse effect during RSI, including episodes of physiologic deterioration. We collected time data from the RSI process by using video review. We explored the association between physician type and first-attempt success.
RESULTS: We obtained complete records for 114 of 123 (93%) children who underwent RSI in the ED during 12 months. Median age was 2.4 years, and 89 (78%) were medical resuscitations. Of the 114 subjects, 59 (52%) were tracheally intubated on the first attempt. Seventy subjects (61%) had 1 or more adverse effects during RSI; 38 (33%) experienced oxyhemoglobin desaturation and 2 required cardiopulmonary resuscitation after physiologic deterioration. Fewer adverse effects were documented in the written records than were observed on video review. The median time from induction through final endotracheal tube placement was 3 minutes. After adjusting for patient characteristics and illness severity, attending-level providers were 10 times more likely to be successful on the first attempt than all trainees combined.
CONCLUSION: Video review of RSI revealed that first-attempt failure and adverse effects were much more common than previously reported for children in an ED.
[/EXPAND]
4. A is for airway: a pediatric emergency department challenge.
Ann Emerg Med. 2012 Sep;60(3):261-3
Reassurance: difficult laryngoscopy in children remains rare
![]() I was taught a useful principle by a paediatric anaesthetist 10 years ago which has proven true in my experience and has contributed to keeping me calm when intubating sick kids. Unlike adults, in whom difficulty in intubation can often be unexpected, the vast majority of normal looking children are easy to intubate, and the ones who are difficult usually have obvious indicators such as dysmorphism.
I was taught a useful principle by a paediatric anaesthetist 10 years ago which has proven true in my experience and has contributed to keeping me calm when intubating sick kids. Unlike adults, in whom difficulty in intubation can often be unexpected, the vast majority of normal looking children are easy to intubate, and the ones who are difficult usually have obvious indicators such as dysmorphism.
This appears to be supported by recent evidence: in a large retrospective series of 11.219 anaesthesia patients, the overall incidence of difficult laryngoscopy [Cormack and Lehane (CML) grade III and IV] was only 1.35%, although was much higher in infants less than one year compared with older children. This low percentage is in the same ball park as two other paediatric studies. Besides younger age, their database suggested underweight, ASA III and IV physical status and, if obtainable, Mallampati III and IV findings as predictors for difficult laryngoscopy. The authors point out:
“…the oromaxillofacial surgery department with a high proportion of cleft palate interventions and pediatric cardiac surgery contributed substantially to the total number of difficult laryngoscopies. In patients undergoing pediatric cardiac surgery, a possible explanation for the higher incidence of CML III/IV findings might be that some congenital heart defects are associated with chromosomal anomalies like microdeletion 22q11.2 syndrome. This syndrome is also associated with extracardiac anomalies like cranio-facial dysmorphism“
Take home message: As a very rough rule of thumb to illustrate the difference between the ease/difficulty of laryngoscopy between adults and kids, I think it’s fair to say grade III or IV views occur in about 10% of adults but only about 1% of children.
Incidence and predictors of difficult laryngoscopy in 11.219 pediatric anesthesia procedures
Paediatr Anaesth. 2012 Aug;22(8):729-36
[EXPAND Click for abstract]
OBJECTIVE: Difficult laryngoscopy in pediatric patients undergoing anesthesia.
AIM: This retrospective analysis was conducted to investigate incidence and predictors of difficult laryngoscopy in a large cohort of pediatric patients receiving general anesthesia with endotracheal intubation.
BACKGROUND: Young age and craniofacial dysmorphy are predictors for the difficult pediatric airway and difficult laryngoscopy. For difficult laryngoscopy, other general predictors are not yet described.
METHODS: Retrospectively, from a 5-year period, data from 11.219 general anesthesia procedures in pediatric patients with endotracheal intubation using age-adapted Macintosh blades in a single center (university hospital) were analyzed statistically.
RESULTS: The overall incidence of difficult laryngoscopy [Cormack and Lehane (CML) grade III and IV] was 1.35%. In patients younger than 1 year, the incidence of CML III or IV was significantly higher than in the older patients (4.7% vs 0.7%). ASA Physical Status III and IV, a higher Mallampati Score (III and IV) and a low BMI were all associated (P < 0.05) with difficult laryngoscopy. Patients undergoing oromaxillofacial surgery and cardiac surgery showed a significantly higher rate of CML III/IV findings.
CONCLUSION: The general incidence of difficult laryngoscopy in pediatric anesthesia is lower than in adults. Our results show that the risk of difficult laryngoscopy is much higher in patients below 1 year of age, in underweight patients and in ASA III and IV patients. The underlying disease might also contribute to the risk. If the Mallampati score could be obtained, prediction of difficult laryngoscopy seems to be reliable. Our data support the existing recommendations for a specialized anesthesiological team to provide safe anesthesia for infants and neonates.
[/EXPAND]
Transtracheal airways in kids. Well, pigs' kids anyway
Ever had to do a surgical airway in a child? Thought not. They’re pretty rare. Bill Heegaard MD from Henepin County Medical Center taught me a few approaches (with the help of an anaesthetised rabbit) which really got me thinking. It’s something I’d often trained for in my internal simulator, and I even keep the equipment for it in my house (listen out for an upcoming podcast on that). Research and experience has demonstrated that open surgical airway techniques are more reliable than transtracheal needle techniques in adults, but what about kids, in whom traditional teaching cautions against open techniques?
Australian investigators who were experienced airway proceduralists evaluated transtracheal needle techniques using a rabbit model (an excellent model for the infant airway). Their success rate was only 60% and they perforated the posterior tracheal wall in 42% of attempts. Of 13 attempts to insert a dedicated paediatric tracheotomy device, the Quicktrach Child, none were successful(1) (they did not use the Quicktrach Infant model as it is not available in Australia).
Danish investigators used fresh piglet cadavers weighing around 8 kg to assess two transtracheal cannulas, in which they achieved success rates of 65.6% and 68.8%(2). There was also a very high rate of posterior tracheal wall perforation. Using an open surgical tracheostomy technique, they were successful in 97% of attempts. These were also experienced operators, with a median anaesthetic experience of 12.5 years.
Their tracheotomy technique was nice and simple, and used just a scalpel, scissors, and surgical towel clips. Here’s their technique:
Simple tracheotomy procedure described by Holm-Knudsen et al
- Identify larynx and proximal trachea by palpation
- Vertical incision through the skin and subcutaneous tissue from the upper part of larynx to the sternal notch
- Grasp strap muscles with two towel forceps and separate in the midline
- Palpate and identify the trachea (palpate rather than look for tracheal rings, as in a live patient one would expect bleeding to obscure the view)
- Stabilise the trachea by grasping it with a towel forceps
- Insert sharp tip of the scissors between two tracheal rings and lift the trachea anteriorly to avoid damage to the posterior wall
- Cut vertically in the midline of the trachea with the scissors – they chose to use the scissors to cut the tracheal rings to facilitate tube insertion
- Insert the tracheal tube
Using ultrasound and CT to evaluate comparative airway dimensions, the authors concluded that the pig model is most useful for training emergency airway management in older children aged 5–10 years.
Why were they doing a tracheotomy rather than a cricothyroidotomy? Reasons given by the authors include:
- The infant cricothyroid membrane is very small
- Palpation of the thyroid notch may be hindered by the overlying hyoid bone
- The mandible may obstruct needle access to the cricothyroid membrane given the cephalad position in the neck of the infant larynx.
From an emergency medicine point of view, there are a couple of other reasons why we need to be able to access the trachea lower than the cricothyroid membrane. One is fractured larynx or other blunt or penetrating airway injury where there may be anatomical disruption at the cricothyroid level. The other situation is foreign body airway obstruction, when objects may lodge at the level of the cricoid ring which is functionally the narrowest part of the pediatric upper airway. Of course, alternative methods might be considered to remove the foreign body prior to tracheotomy, such as employing basic choking algorithms, and other techniques depending on whether you do or don’t have equipment.
Take home messages
- Transtracheal airways in kids are so rare, we can’t avoid extrapolating animal data
- Whichever infant or paediatric model is used, transtracheal needle techniques have a high rate of failure even by ‘experienced’ operators
- The small size and easy compressibility of the airway probably contributes to this failure rate, including the high rate of posterior wall puncture
- In keeping with adult audit data, open surgical techniques may have a higher success rate
- Tracheotomy may be necessary rather than cricothyroidotomy in infants and children depending on clinical scenario and accessibility of anatomy
- The stress and blood that is not simulated in cadaveric animal models will make open tracheotomy harder in a live patient, and so these success rates may not translate. However these factors do mean that whatever technique is used must be kept simple and should employ readily available and familiar equipment
- Something to maintain control and anterior position of the anterior trachea wall should be used during incision and intubation of the trachea. The study reported here used towel clips; sutures around the tracheal rings may also be used (see image below)
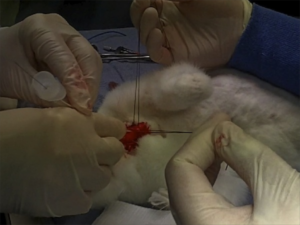
I recommend you add ‘paediatric tracheotomy’ to the list of procedures you might need to do (if it’s not already there). Identify what equipment you would use and run the simulation in your head and in your work environment.
Have fun.
1. The ‘Can’t Intubate Can’t Oxygenate’ scenario in Pediatric Anesthesia: a comparison of different devices for needle cricothyroidotomy
Paediatr Anaesth. 2012 Dec;22(12):1155-8
BACKGROUND: Little evidence exists to guide the management of the ‘Can’t Intubate, Can’t Oxygenate’ (CICO) scenario in pediatric anesthesia.
OBJECTIVES: To compare two intravenous cannulae for ease of use, success rate and complication rate in needle tracheotomy in a postmortem animal model of the infant airway, and trial a commercially available device using the same model.
METHODS: Two experienced proceduralists repeatedly attempted cannula tracheotomy in five postmortem rabbits, alternately using 18-gauge (18G) and 14-gauge (14G) BD Insyte(™) cannulae (BD, Franklin Lakes, NJ, USA). Attempts began at the first tracheal cartilage, with subsequent attempts progressively more caudad. Success was defined as intratracheal cannula placement. In each rabbit, an attempt was then made by each proceduralist to perform a cannula tracheotomy using the Quicktrach Child(™) device (VBM Medizintechnik GmbH, Sulz am Neckar, Germany).
RESULTS: The rabbit tracheas were of similar dimensions to a human infant. 60 attempts were made at cannula tracheotomy, yielding a 60% success rate. There was no significant difference in success rate, ease of use, or complication rate between cannulae of different gauge. Successful aspiration was highly predictive (positive predictive value 97%) and both sensitive (89%) and specific (96%) for tracheal cannulation. The posterior tracheal wall was perforated in 42% of tracheal punctures. None of 13 attempts using the Quicktrach Child(™) were successful.
CONCLUSION: Cannula tracheotomy in a model comparable to the infant airway is difficult and not without complication. Cannulae of 14- and 18-gauge appear to offer similar performance. Successful aspiration is the key predictor of appropriate cannula placement. The Quicktrach Child was not used successfully in this model. Further work is required to compare possible management strategies for the CICO scenario
2. Emergency airway access in children – transtracheal cannulas and tracheotomy assessed in a porcine model
Paediatr Anaesth. 2012 Dec;22(12):1159-65
OBJECTIVES: In the rare scenario when it is impossible to oxygenate or intubate a child, no evidence exists on what strategy to follow.
AIM: The aim of this study was to compare the time and success rate when using two different transtracheal needle techniques and also to measure the success rate and time when performing an emergency tracheotomy in a piglet cadaver model.
METHODS: In this randomized cross-over study, we included 32 anesthesiologists who each inserted two transtracheal cannulas (TTC) using a jet ventilation catheter and an intravenous catheter in a piglet model. Second, they performed an emergency tracheotomy. A maximum of 2 and 4 min were allowed for the procedures, respectively. The TTC procedures were recorded using a video scope.
RESULTS: Placement of a transtracheal cannula was successful in 65.6% and 68.8% of the attempts (P = 0.76), and the median duration of the attempts was 69 and 42 s (P = 0.32), using the jet ventilation catheter and the intravenous catheter, respectively. Complications were frequent in both groups, especially perforation of the posterior tracheal wall. Performing an emergency tracheotomy was successful in 97%, in a median of 88 s.
CONCLUSIONS: In a piglet model, we found no significant difference in success rates or time to insert a jet ventilation cannula or an intravenous catheter transtracheally, but the incidence of complications was high. In the same model, we found a 97% success rate for performing an emergency tracheotomy within 4 min with a low rate of complications.
Don't bronchodilators work in infants?
Inpatient paediatric teams can be scornful when bronchodilators are given by ED staff to wheezing infants, correctly referring to the lack of evidence of clinical benefit(1). There is however a persisting meme out there I’ve heard on a number of occasions that ‘young infants don’t have the receptors so inhaled beta agonists will never work.’ I’d love to know where this comes from.
Apparently, beta 2-receptors are present from the 16th gestational week(2). Pulmonary function testing of ventilated, very-low-birth-weight babies has shown that some consistently responded to beta-agonists whereas others did not(3). A newly published study reports that a quarter of mechanically ventilated infants with bronchiolitis were responders to inhaled albuterol, defined as a reduction in respiratory system resistance more than 30% below baseline(4).
In summary: beta-agonist bronchodilators have not been shown to improve clinical outcomes in wheezing infants. However some infants with some wheezing disorders will show a response in terms of pulmonary function. The receptors are there, and in life-threatening presentations bronchodilators should certainly be considered.
1. Short acting beta agonists for recurrent wheeze in children under 2 years of age
Cochrane Database Syst Rev. 2002;(3):CD002873
[EXPAND Click to read abstract]
BACKGROUND: Wheeze is a common symptom in infancy and is a common cause for both primary care consultations and hospital admission. Beta2-adrenoceptor agonists (b2-agonists) are the most frequently used as bronchodilator but their efficacy is questionable.
OBJECTIVES: To determine the effectiveness of b2-agonist for the treatment of infants with recurrent and persistent wheeze.
SEARCH STRATEGY: Relevant trials were identified using the Cochrane Airways Group database (CENTRAL), Medline and Pubmed. The database search used the following terms: Wheeze or asthma and Infant or Child and Short acting beta-agonist or Salbutamol (variants), Albuterol, Terbutaline (variants), Orciprenaline, Fenoterol
SELECTION CRITERIA: Randomised controlled trials comparing the effect of b2-agonist against placebo in children under 2 years of age who had had two or more previous episodes of wheeze, not related to another form of chronic lung disease.
DATA COLLECTION AND ANALYSIS: Eight studies met the criteria for inclusion in this meta-analysis. The studies investigated patients in three settings: at home (3 studies), in hospital (2 studies) and in the pulmonary function laboratory (3 studies). The main outcome measure was change in respiratory rate except for community based studies where symptom scores were used.
MAIN RESULTS: The studies were markedly heterogeneous and between study comparisons were limited. Improvement in respiratory rate, symptom score and oxygen saturation were noted in one study in the emergency department following two salbutamol nebulisers but this had no impact on hospital admission. There was a reduction in bronchial reactivity following salbutamol. There was no significant benefit from taking regular inhaled salbutamol on symptom scores recorded at home.
REVIEWER’S CONCLUSIONS: There is no clear benefit of using b2-agonists in the management of recurrent wheeze in the first two years of life although there is conflicting evidence. At present, further studies should only be performed if the patient group can be clearly defined and there is a suitable outcome parameter capable of measuring a response.
[/EXPAND]
2. The beta-2-agonists in asthma in infants and young children
Arch Pediatr. 2002 Aug;9 Suppl 3:384s-389s
[EXPAND Click to read abstract]
Beta 2-agonists, by inducing a fast and long relaxation of the bronchial smooth muscle, are considered as the more potent bronchodilators. beta 2-receptors are present from the 16th gestational week, explaining a possible bronchial response in the youngest children. beta 2-agonists do not induce any bronchodilator response in healthy children. Short-acting beta 2-agonists (salbutamol or albuterol, terbutaline) are indicated for asthma attacks, as needed in chronic asthma, and for prevention of symptoms during effort. They are safe and secure. The more efficient route of administration in preschool children is pressurized metered-dose inhaler used with a spacer device. Therefore, whatever the route of inhalation chosen (inhalation, injection, or continuous nebulization in acute asthma attack), more specified indications and doses are needed in young children. Long-acting beta 2-agonists (formoterol, salmeterol) are not authorized in France in children under 4 to 5 years of age depending on the drug used. Because of new oral formulations and recent considerations about their use in asthma attack, instead of short-acting beta 2-agonists, their indication in preschool asthmatic children might be reconsidered.
[/EXPAND]
3. Use of a beta-agonist in ventilated, very-low-birth-weight babies: a longitudinal evaluation
Dev Pharmacol Ther. 1990;15(2):61-7
[EXPAND Click to read abstract]
To determine if there is a specific postnatal (PNA) or postconceptional age (PCA) at which ventilated preterm infants respond to beta-agonists, we evaluated 15 infants with a mean gestational age of 26.5 +/- 1.5 weeks and mean birth weight of 0.89 +/- 0.23 kg who required mechanical ventilation at 10 days of age. Weekly pulmonary function testing (PFT) was performed before and 1 h after administration of albuterol. Taking the group as a whole, as well as individual babies, regression analysis showed no relationship between positive response and either PNA or PCA. Evaluation of individual infants, however, showed that some consistently responded to beta-agonists whereas others did not. We recommend individual PFT to identify those infants who will benefit from use of beta-agonists.
[/EXPAND]
4. Pulmonary mechanics following albuterol therapy in mechanically ventilated infants with bronchiolitis
J Asthma. 2012 Sep;49(7):688-96
[EXPAND Click to read abstract]
BACKGROUND AND AIMS: Bronchiolitis is a common cause of critical illness in infants. Inhaled β(2)-agonist bronchodilators are frequently used as part of treatment, despite unproven effectiveness. The purpose of this study was to describe the physiologic response to these medications in infants intubated and mechanically ventilated for bronchiolitis.
MATERIALS AND METHODS: We conducted a prospective trial of albuterol treatment in infants intubated and mechanically ventilated for bronchiolitis. Before and for 30 minutes following inhaled albuterol treatment, sequential assessments of pulmonary mechanics were determined using the interrupter technique on repeated consecutive breaths.
RESULTS: Fifty-four infants were enrolled. The median age was 44 days (25-75%; interquartile range (IQR) 29-74 days), mean hospital length of stay (LOS) was 18.3 ± 13.3 days, mean ICU LOS was 11.3 ± 6.4 days, and mean duration of mechanical ventilation was 8.5 ± 3.5 days. Fifty percent (n = 27) of the infants were male, 81% (n = 44) had public insurance, 80% (n = 41) were Caucasian, and 39% (n = 21) were Hispanic. Fourteen of the 54 (26%) had reduction in respiratory system resistance (Rrs) that was more than 30% below baseline, and were defined as responders to albuterol. Response to albuterol was not associated with demographic factors or hospitalization outcomes such as LOS or duration of mechanical ventilation. However, increased Rrs, prematurity, and non-Hispanic ethnicity were associated with increased LOS.
CONCLUSIONS: In this population of mechanically ventilated infants with bronchiolitis, relatively few had a reduction in pulmonary resistance in response to inhaled albuterol therapy. This response was not associated with improvements in outcomes.
[/EXPAND]
ECMO for paediatric cardiac arrest
The Taiwanese are at it again with their extracorporeal life support. This time, they report their outcomes in children who received ECMO for in-hospital cardiac arrest. Interestingly, the patients with pure cardiac causes of cardiac arrest had a survival rate similar to patients with non-cardiac causes.
PURPOSE: The study aims to describe 11 years of experience with extracorporeal cardiopulmonary resuscitation (ECPR) for in-hospital paediatric cardiac arrest in a university affiliated tertiary care hospital.
METHODS: Paediatric patients who received extracorporeal membrane oxygenation (ECMO) during active extracorporeal cardiopulmonary resuscitation (ECPR) at our centre from 1999 to 2009 were included in this retrospective study. The results from three different cohorts (1999-2001, 2002-2005 and 2006-2009) were compared. Survival rates and neurological outcomes were analysed. Favourable neurological outcome was defined as paediatric cerebral performance categories (PCPC) 1, 2 and 3.
RESULTS: We identified 54 ECPR events. The survival rate to hospital discharge was 46% (25/54), and 21 (84%) of the survivors had favourable neurological outcomes. The duration of CPR was 39±17 min in the survivors and 52±45 min in the non-survivors (p=NS). The patients with pure cardiac causes of cardiac arrest had a survival rate similar to patients with non-cardiac causes (47% (18/38) vs. 44% (7/16), p=NS). The non-survivors had higher serum lactate levels prior to ECPR (13.4±6.4 vs. 8.8±5.1 mmol/L, p<0.01) and more renal failure after ECPR (66% (19/29) vs. 20% (5/25), p<0.01). The patients resuscitated between 2006 and 2009 had shorter durations of CPR (34±13 vs. 78±76 min, p=0.032) and higher rates of survival (55% (16/29) vs. 0% (0/8), p=0.017) than those resuscitated between 1999 and 2002.
CONCLUSIONS: In our single-centre experience with ECPR for paediatric in-hospital cardiac arrest, the duration of CPR has become shorter and outcomes have improved in recent years. Higher pre-ECPR lactate levels and the presence of post-ECPR renal failure were associated with increased mortality. The presence of non-cardiac causes of cardiac arrest did not preclude successful ECPR outcomes. The duration of CPR was not significantly associated with poor outcomes in this study.
Eleven years of experience with extracorporeal cardiopulmonary resuscitation for paediatric patients with in-hospital cardiac arrest
Resuscitation. 2012 Jun;83(6):710-4
Hypotonic Versus Isotonic Fluids After Surgery for Children
Kids in hospital with injury, infection or other illness, and those undergoing the physiological stress of surgery, produce (appropriately) elevated antidiuretic hormone levels which contribute to the risk of hyponatraemia by impairing free water excretion in the kidney.
Deaths have occurred on general paediatric and surgery wards when fluid regimens containing low concentrations of sodium (classically 0.18% or 0.225% NaCl) have resulted in hyponatraemia in children without adequate electrolyte monitoring, leading some bodies to recommend at least 0.45% NaCl solutions for maintenance fluid therapy in children.
However two recent studies1,2 on postoperative children show an increased risk of hyponatraemia even with 0.45% saline, when compared with 0.9% saline or Hartmann’s solution (Hartmann’s is similar – almost identical – to Ringer’s lactate).
I like the fact that paediatricians used Hartmann’s in one of these studies1. I have worked with several paediatricians who never use Hartmann’s, either from lack of experience or because of concern about its lactate content (not appreciating the lactate is metabolised by the liver to bicarbonate).
This is ironic, since Alexis Hartmann (1898–1964) was a paediatrician.
Want more fluid therapy irony? The ‘balanced salt solution’ used by Brits and Australasians is Hartmann’s solution – named after an American. The one used by Americans is Lactated Ringer’s solution – named after the British physician Sydney Ringer (1834-1910).
Medical history enthusiasts can read more about Hartmann and Ringer here.
1. A randomised controlled trial of Hartmann’s solution versus half normal saline in postoperative paediatric spinal instrumentation and craniotomy patients.
Arch Dis Child. 2012 Jun;97(6):491-6
[EXPAND Click to read abstract]
OBJECTIVE: To compare the difference in plasma sodium at 16-18 h following major surgery in children who were prescribed either Hartmann’s and 5% dextrose or 0.45% saline and 5% dextrose.
DESIGN: A prospective, randomised, open label study.
SETTING: The paediatric intensive care unit (650 admissions per annum) in a tertiary children’s hospital in Brisbane, Australia.
PATIENTS: The study group comprised 82 children undergoing spinal instrumentation, craniotomy for brain tumour resection, or cranial vault remodelling.
INTERVENTIONS: Patients received either Hartmann’s and 5% dextrose at full maintenance rate or 0.45% saline and 5% dextrose at two-thirds maintenance rate.
MAIN OUTCOMES MEASURES: Primary outcome measure: plasma sodium at 16-18 h postoperatively; secondary outcome measure: number of fluid boluses administered.
RESULTS: Mean postoperative plasma sodium levels of children receiving 0.45% saline and 5% dextrose were 1.4 mmol/l (95% CI 0.4 to 2.5) lower than those receiving Hartmann’s and 5% dextrose (p=0.008). In the 0.45% saline group, seven patients (18%) became hyponatraemic (Na <135 mmol/l) at 16-18 h postoperatively; in the Hartmann’s group no patient became hyponatraemic (p=0.01). No child in either fluid group became hypernatraemic.
CONCLUSIONS: The postoperative fall in plasma sodium was smaller in children who received Hartmann’s and 5% dextrose compared to those who received 0.45% saline and 5% dextrose. It is suggested that Hartmann’s and 5% dextrose should be administered at full maintenance rate postoperatively to children who have undergone major surgery in preference to hypotonic fluids.
[/EXPAND]
2. Hypotonic versus isotonic maintenance fluids after surgery for children: a randomized controlled trial
Pediatrics. 2011 Nov;128(5):857-66.
[EXPAND Click to read abstract]
OBJECTIVE: The objective of this randomized controlled trial was to evaluate the risk of hyponatremia following administration of a isotonic (0.9% saline) compared to a hypotonic (0.45% saline) parenteral maintenance solution (PMS) for 48 hours to postoperative pediatric patients.
METHODS: Surgical patients 6 months to 16 years of age with an expected postoperative stay of >24 hours were eligible. Patients with an uncorrected baseline plasma sodium level abnormality, hemodynamic instability, chronic diuretic use, previous enrollment, and those for whom either hypotonic PMS or isotonic PMS was considered contraindicated or necessary, were excluded. A fully blinded randomized controlled trial was performed. The primary outcome was acute hyponatremia. Secondary outcomes included severe hyponatremia, hypernatremia, adverse events attributable to acute plasma sodium level changes, and antidiuretic hormone levels.
RESULTS: A total of 258 patients were enrolled and assigned randomly to receive hypotonic PMS (N = 130) or isotonic PMS (N = 128). Baseline characteristics were similar for the 2 groups. Hypotonic PMS significantly increased the risk of hyponatremia, compared with isotonic PMS (40.8% vs 22.7%; relative risk: 1.82 [95% confidence interval: 1.21-2.74]; P = .004). Admission to the pediatric critical care unit was not an independent risk factor for the development of hyponatremia. Isotonic PMS did not increase the risk of hypernatremia (relative risk: 1.30 [95% confidence interval: 0.30-5.59]; P = .722). Antidiuretic hormone levels and adverse events were not significantly different between the groups.
CONCLUSION: Hypotonic Versus Isotonic Maintenance Fluids After Surgery for Children: A Randomized Controlled Trial.
[/EXPAND]
Not a pin cushion
This is the daughter of my friend. Avery is only seven months old and has survived a critical illness and is thankfully now fully recovered. Her Dad has nothing but praise for the medical and nursing staff who cared for her. But one thing could have been better. Avery endured multiple attempts at vascular access without ultrasound guidance.
If you were her parent, and you were an emergency physician with galaxy-class expertise in emergency ultrasound, how would you react? Complaints? Incident forms? Outrage?
How about education? For free. Accompanied by lavish praise for the experts who treated Avery and made her better.
Avery’s Dad is ultrasound podcaster and gentleman Dr Matt Dawson. He is offering FREE ultrasound training to anyone who wants to improve their vascular access skills.
Are there nurses, physicians, or technicians in your ED or ICU that could improve their care with this training? Please consider sending them for this training. To register for the course, and to read Avery’s full story, go to notapincushion.com.
And if you’re already comfortable with ultrasound-guided vascular access, then visit the site anyway, as there is some education here for all of us: how to turn a gut-wrenchingly distressing experience into something positive that will benefit countless others. I am thoroughly inspired.
Best wishes to an amazing family.
Cliff
Out-of hospital traumatic paediatric cardiac arrest
This small study on traumatic arrests in children1 refutes the “100% mortality from traumatic arrest” dogma that people still spout and gives information on the mechanisms associated with survival: drowning and strangulation were associated with greater rates of survival to hospital admission compared with blunt, penetrating, and other traumas. Overall, drowning had the greatest rate of survival to discharge (19.1%).
I would like to know the injuries sustained in non-survivors, to determine whether they were potentially treatable. Strikingly, in the list of prehospital procedures performed, there were NO attempts at pleural decompression, something that is standard in traumatic arrest protocols in prehospital services were I have worked.
It is interesting to compare these results with those of the London HEMS team2, who for traumatic paediatric arrest achieved 19/80 (23.8%) survival to discharged from the emergency department and 7/80 (8.75%) survival to hospital discharge. They also noted a large proportion of the survivors suffered hypoxic or asphyxial injuries, whereas those patients with hypovolaemic cardiac arrest did not survive.
OBJECTIVE:To determine the epidemiology and survival of pediatric out-of-hospital cardiac arrest (OHCA) secondary to trauma.
METHODS:The CanAm Pediatric Cardiac Arrest Study Group is a collaboration of researchers in the United States and Canada sharing a common goal to improve survival outcomes for pediatric cardiac arrest. This was a prospective, multicenter, observational study. Twelve months of consecutive data were collected from emergency medical services (EMS), fire, and inpatient records from 2000 to 2003 for all OHCAs secondary to trauma in patients aged ≤18 years in 36 urban and suburban communities supporting advanced life support (ALS) programs. Eligible patients were apneic and pulseless and received chest compressions in the field. The primary outcome was survival to discharge. Secondary measures included return of spontaneous circulation (ROSC), survival to hospital admission, and 24-hour survival.
RESULTS:The study included 123 patients. The median patient age was 7.3 years (interquartile range [IQR] 6.0-17.0). The patient population was 78.1% male and 59.0% African American, 20.5% Hispanic, and 15.7% white. Most cardiac arrests occurred in residential (47.1%) or street/highway (37.2%) locations. Initial recorded rhythms were asystole (59.3%), pulseless electrical activity (29.1%), and ventricular fibrillation/tachycardia (3.5%). The majority of cardiac arrests were unwitnessed (49.5%), and less than 20% of patients received chest compressions by bystanders. The median (IQR) call-to-arrival interval was 4.9 (3.1-6.5) minutes and the on-scene interval was 12.3 (8.4-18.3) minutes. Blunt and penetrating traumas were the most common mechanisms (34.2% and 25.2%, respectively) and were associated with poor survival to discharge (2.4% and 6.5%, respectively). For all OHCA patients, 19.5% experienced ROSC in the field, 9.8% survived the first 24 hours, and 5.7% survived to discharge. Survivors had triple the rate of bystander cardiopulmonary resuscitation (CPR) than nonsurvivors (42.9% vs. 15.2%). Unlike patients sustaining blunt trauma or strangulation/hanging, most post-cardiac arrest patients who survived the first 24 hours after penetrating trauma or drowning were discharged alive. Drowning (17.1% of cardiac arrests) had the highest survival-to-discharge rate (19.1%).
CONCLUSIONS:The overall survival rate for OHCA in children after trauma was low, but some trauma mechanisms are associated with better survival rates than others. Most OHCA in children is preventable, and education and prevention strategies should focus on those overrepresented populations and high-risk mechanisms to improve mortality.
1. Epidemiology of out-of hospital pediatric cardiac arrest due to trauma
Prehosp Emerg Care, 2012 vol. 16 (2) pp. 230-236
2. Outcome from paediatric cardiac arrest associated with trauma
Resuscitation. 2007 Oct;75(1):29-34
Passive leg raise predicted fluid responsiveness in kids
Passive leg raising (PLR) is a great ‘free reversible fluid challenge’ to see if a shocked or hypotensive patient is likely to respond to volume therapy. A new study assesses its applicability in children.
PLR predicted fluid responders with 85% specificity but a lack of response did not rule out fluid responsiveness. Also, the effect of the PLR on cardiac index measured by echocardiography was the only way of predicting response – there was no relation to the more easily monitored effects of PLR on systolic blood pressure or heart rate.
Want to learn how to measure cardiac output using ultrasound? Mike Mallin from the Emergency Ultrasound Podcast shows you how here
OBJECTIVE: Fluid challenge is often used to predict fluid responsiveness in critically ill patients. Inappropriate fluid expansion can lead to some unwanted side effects; therefore, we need a noninvasive predictive parameter to assess fluid responsiveness. We want to assess the hemodynamic parameter changes after passive leg raising, which can mimic fluid expansion, to predict fluid responsiveness in pediatric intensive care unit patients and to get a cutoff value of cardiac index in predicting fluid responsiveness in pediatric patients.
DESIGN: Nonrandomized experimental study.
SETTING: Tertiary academic pediatric intensive care.
PATIENTS: Children admitted to pediatric intensive care.
INTERVENTION: Hemodynamic parameters were assessed at baseline, after passive leg raising, at second baseline, and after volume expansion (10 mL/kg normal saline infusion over 15 mins).
MEASUREMENTS AND MAIN RESULTS: We measured the heart rate, systolic blood pressure, and stroke volume and cardiac index using Doppler echocardiography. The hemodynamic parameter changes induced by passive leg raising were monitored. Among 40 patients included in the study, 20 patients had a cardiac index increase of ≥10% after volume expansion (responders). Changes in heart rate, systolic blood pressure, and stroke volume after passive leg raising did not significantly relate to the response to volume expansion. There was significant relation between changes in cardiac index to predict fluid responsiveness (p = .012, r = .22, 95% confidence interval 1.529 to 31.37). A cardiac index increase by ≥10% induced by passive leg raising predicted preload-dependent status with sensitivity of 55% and specificity of 85% (area under the curve 0.71 ± 0.084, 95% confidence interval 0.546-0.874).
CONCLUSION: The concomitant measurements in cardiac index changes after the passive leg raising maneuver can be helpful in predicting who might have an increase in cardiac index with subsequent fluid resuscitation.
The role of passive leg raising to predict fluid responsiveness in pediatric intensive care unit patients.
Pediatric Critical Care Medicine. 13(3):e155-e160, May 2012


