Can cardiotocography be applied in the pre-hospital setting? French physicians assessed its feasibility in 145 patients enrolled during 119 interhospital transfers and 26 primary prehospital missions.
Their physician-staffed ambulance teams included 19 emergency physicians and one anaesthetist.
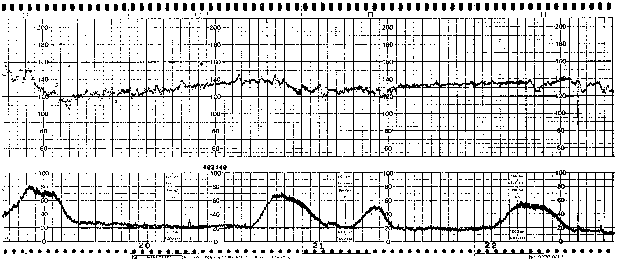
Interpretable tracings were obtained for 81% of the patients during the initial examination, but this rate decreased to 66% during handling and transfer procedures. Only ground EMS transportations were included in the study. For 17 patients (12%), the monitoring led to a change in the patient’s management: an acceleration of chronology of prehospital management in 5 cases, a decision to directly admit the patient to the operating room for immediate cesarean section in three cases, a change in hospital admission in three cases, an adaptation or implementation of tocolytic treatment in six cases, and placing the patient in the left lateral decubitus position or oxygen administration in three cases.
Fetal monitoring in the prehospital setting
J Emerg Med. 2010 Nov;39(5):623-8
Tag Archives: pregnancy
A-a gradient unhelpful in pregnancy
Given that thromboembolism is the leading cause of maternal death in the UK according to the latest UK CEMACE report, it would be nice to have reliable non-ionising tests in the ED to rapidly rule out this disease in pregnant women. Unfortunately, the alveolar-arterial oxygen gradient does not do the job.
A recent study compared the A-a gradient with CTPA as the gold standard. Of 102 patients who were pregnant or up to 6 weeks post-partum, there were 13 PEs (2 antepartum and 11 postpartum). The best sensitivity, specificity, and negative and positive predictive values for A-a gradients were 76.9%, 20.2%, 80.0%, and 11.5%, respectively.
Assessment of the alveolar-arterial oxygen gradient as a screening test for pulmonary embolism in pregnancy
Am J Obstet Gynecol. 2010 Oct;203(4):373.e1-4
Imaging for PE in pregnancy
A review article on pulmonary embolism in pregnancy reminds us that the mortality associated with untreated PE far outweighs the potential oncogenic and teratogenic risk incurred by fetal exposure to diagnostic imaging for PE.
Teratogenicity
The minimum dose of radiation associated with increased risk of teratogenicity in human beings has yet to be firmly established, but on the basis of compiled mouse, rat, and human data, radiation exposure of 0·1 Gy at any time during gestation is regarded as a practical threshold beyond which induction of congenital abnormalities is possible.
Oncogenicity
An exposure of the conceptus to 0·01 Gy above natural background radiation increases the probability of cancer before the age of 20 years from 0·03% to 0·04%.
Reassuringly, a chest radiograph, ventilation perfusion scan, and conventional pulmonary angiogram combined with CT pulmonary angiogram expose the fetus to a total of 0·004 Gy.
Pulmonary embolism in pregnancy
Lancet. 2010 Feb 6;375(9713):500-12
Fetal ultrasound safe
From the UK’s Health Protection Agency website:
The independent Advisory Group on Non-Ionising Radiation (AGNIR), which reports to the Health Protection Agency, has reviewed the latest scientific evidence on the health effects of ultrasound (frequencies above 20 kilohertz) and infrasound (below 20 Hz).
The report finds that the available evidence does not suggest that diagnostic ultrasound affects mortality of babies during pregnancy or soon after birth. The evidence also does not suggest any effect on childhood cancer risk. There have, however, been some unconfirmed reports suggesting possible effects on the developing nervous system – for instance, on handedness of the child.
AGNIR concluded that there is no established evidence that diagnostic levels of ultrasound are hazardous. However, further research is needed to determine whether there are any long-term adverse health effects, especially following exposure of the unborn child.
Asthma guidelines (in pregnancy) 2009 revision
A reminder of the British Thoracic Society guidelines on the management of asthma, revised June 2009

