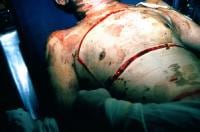
A military study revealed troops suffering from severe burns tended to receive either no prehospital fluid or too much fluid1.
The authors point out some practical realities and an attempted solution:
For a medic potentially treating multiple casualties at once in a hostile environment, the calculation of the modified Brooke or Parkland formula may be unrealistic prior to beginning fluid resuscitation in the prehospital setting.
The USAISR’s Rule of 10 is a simplified formula to guide the initial fluid resuscitation of a burn victim. The burn size is estimated to the nearest 10% TBSA. For patients weighing 40 to 80 kg, the burn size is then multiplied by 10 to give the initial fluid rate in milliliters per hour. The rate is increased by 100 mL/hour for every 10 kg above 80 kg in terms of the patient’s weight. For the majority of adult burn patients, the Rule of 10 approximates the initial fluid rate within accepted ABA guidelines.
A previous study on the rule of 10 showed it provided an estimate that fell between the modified Brooke and Parkland estimates 87.8% of the time, less than the modified Brooke <12% of the time, and hardly ever (>1%) exceeded the Parkland estimate2.
OBJECTIVE: The purpose of this article is to provide a descriptive study of the management of burns in the prehospital setting of a combat zone.
METHODS: A retrospective chart review was performed of U.S. casualties with >20% total-body-surface-area thermal burns, transported from the site of injury to Ibn Sina Combat Support Hospital (CSH) between January 1, 2006, and August 30, 2009.
RESULTS: Ibn Sina CSH received 225 burn casualties between January 2006 and August 2009. Of these, 48 met the inclusion criteria. The mean Injury Severity Score was 31.7 (range 4 to 75). Prehospital vascular access was obtained in 24 casualties (50%), and 20 of the casualties received fluid resuscitation. Out of the 48 casualties enrolled, 28 (58.3%) did not receive prehospital fluid resuscitation. Of the casualties who received fluid resuscitation, nearly all received volumes in excess of the guidelines established by the American Burn Association and those recommended by the Committee for Tactical Combat Casualty Care. With regard to pain management in the prehospital setting, 13 casualties (27.1%) received pain medication.
CONCLUSIONS: With regard to the prehospital fluid resuscitation of primary thermal injury in the combat zone, two extremes were noted. The first group did not receive any fluid resuscitation; the second group was resuscitated with fluid volumes higher than those expected if established guidelines were utilized. Pain management was not uniformly provided to major burn casualties, even in several with vascular access. These observations support improved education of prehospital personnel serving in a combat zone.
1. Prehospital burn management in a combat zone
Prehosp Emerg Care, 2012 vol. 16 (2) pp. 273-276
2. Simple derivation of the initial fluid rate for the resuscitation of severely burned adult combat casualties: in silico validation of the rule of 10
J Trauma. 2010 Jul;69 Suppl 1:S49-54