The current mortality of 35% associated with acute lung injury (ALI) is roughly three times higher than that associated with ST-segment elevation myocardial infarction. Protective ventilation strategies limiting tidal volumes and plateau pressures improve outcome, but the optimial level of PEEP is debated. In patients with ALI and its more severe form acute respiratory distress syndrome (ARDS), higher levels of PEEP may prevent atelectasis, recruit already collapsed alveolar units, and reduce pulmonary damage by avoiding the cyclical opening and collapse of alveoli.
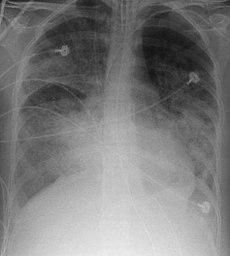
In a systematic review and meta-analysis of individual-patient data, researchers investigated the association between higher vs lower PEEP levels and patient-important outcomes among adults with acute lung injury or ARDS who receive ventilation with low tidal volumes.
Randomized trials eligible for this review compared higher with lower levels of PEEP (mean difference of at least 3 cm H2O between groups) in critically ill adults with ALI or ARDS. Eligible trials incorporated a target tidal volume of less than 8 mL/kg of predicted body weight in both the experimental and the control ventilation strategies and provided patient follow-up to death or for at least 20 days.

Three trials, including 2299 patients, met the eligibility criteria: the Assessment of Low Tidal Volume and Elevated End-Expiratory Pressure to Obviate Lung Injury (ALVEOLI) trial, the Lung Open Ventilation to Decrease Mortality in the Acute Respiratory Distress Syndrome (LOVS) study, and the Expiratory Pressure Study (EXPRESS).
There were 374 hospital deaths in 1136 patients (32.9%) assigned to treatment with higher PEEP and 409 hospital deaths in 1163 patients (35.2%) assigned to lower PEEP (adjusted relative risk [RR], 0.94; 95% confidence interval [CI], 0.86-1.04; P = .25). Treatment effects varied with the presence or absence of ARDS (as opposed to ALI). In patients with ARDS (n = 1892), there were 324 hospital deaths (34.1%) in the higher PEEP group and 368 (39.1%) in the lower PEEP group (adjusted RR, 0.90; 95% CI, 0.81-1.00; P = .049). Rates of pneumothorax and vasopressor use were similar.
The authors conclude that treatment with higher vs lower levels of PEEP was not associated with improved hospital survival overall when ALI/ARDS were considered together, but higher levels were associated with improved survival among the pre-defined subgroup of patients with ARDS.
Higher vs lower positive end-expiratory pressure in patients with acute lung injury and acute respiratory distress syndrome: systematic review and meta-analysis
JAMA. 2010 Mar 3;303(9):865-73
Tag Archives: ventilation
Difficult mask ventilation
A comprehensive review of difficult mask ventilation (DMV) reports that the incidence of DMV varies widely (from 0.08% to 15%) depending on the criteria used for its definition. It reminds us that the independent predictors of DMV are:
- Obesity
- Age older than 55 yr
- History of snoring
- Lack of teeth
- The presence of a beard
- Mallampati Class III or IV
- Abnormal mandibular protrusion test
The review also points out that DMV does not automatically mean difficult laryngoscopy, although it does increase its likelihood.
In addition to positioning, oral and nasal adjuncts, two person technique, and jaw thrust, the application of 10 cmH20 CPAP may help splint open the airway and reduce the difficulty of mask ventilation in some patients.
Difficult mask ventilation
Anesth Analg. 2009 Dec;109(6):1870-80
Causes of DMV:
1) Technique-related
1. Operator: Lack of experience
2. Equipment
a. Improper mask size
b. Difficult mask fit: e.g., beard, facial anomalies, retrognathia
c. Leakage from the circuit
d. Faulty valve
e. Improper oral/nasal airway size
3. Position: Suboptimal head and neck position
4. Incorrectly applied cricoid pressure
5. Drug related
a. Opioid-induced vocal cord closure
b. Succinylcholine-induced masseter rigidity
c. Inadequate depth of anesthesia
d. Lack of relaxation?
2) Airway-related
1. Upper airway obstruction
a. Tongue or epiglottis
b. Redundant soft tissue in morbid obesity and sleep
apnea patients
c. Tonsillar hyperplasia
d. Oral, maxillary, pharyngeal, or laryngeal tumor
e. Airway edema e.g., repeated intubation attempts,
trauma, angioedema
f. Laryngeal spasm
g. External compression e.g., large neck masses and
neck hematoma
2. Lower airway obstruction
a. Severe bronchospasm
b. Tracheal or bronchial tumor
c. Anterior mediastinal mass
d. Stiff lung
e. Foreign body
f. Pneumothorax
g. Bronchopleural fistula
3) Severe chest wall deformity or kyphoscoliosis restricting chest expansion
Prehospital Hypocapnia and Poor Outcome After Severe Traumatic Brain Injury
Patients admitted to a level 1 trauma centre with traumatic brain injury whose end-tidal CO2 was kept with the Brain Trauma Foundation recommended limits of 30-35 mmHg (3.9-4.6 kPa) had a lower mortality than those whose CO2 was outside this range. The group in which the target was not achieved had a greater injury severity, which may have contribute to the difficulty in optimising ETCO2.
Prehospital Hypocapnia and Poor Outcome After Severe Traumatic Brain Injury
J Trauma. 2009 Jun;66(6):1577-82
Paeds BVM for adult resus
Smaller self-inflating bags produce greater guideline consistent ventilation in simulated cardiopulmonary resuscitation
A comparison between two sizes of self-inflating resuscitation bags revealed improved adherence to resuscitation guidelines with the smaller bag. Student paramedics were more likely to produce suboptimal tidal volumes and ventilation rates with a 1500ml bag than a 1000ml bag during simulated ventilation of an artificial lung model.
BMC Emerg Med. 2009 Feb 20;9:4
http://www.ncbi.nlm.nih.gov/pubmed/19228432
Full text at http://www.biomedcentral.com/1471-227X/9/4
NIV for weaning
Use of non-invasive ventilation to wean critically ill adults off invasive ventilation: meta-analysis and systematic review
The growing evidence base in support of liberating patients from invasive mechanical ventilation by means of non-invasive weaning is summarised in this systematic review of 12 randomised trials. Non-invasive weaning was associated with decreased mortality, ventilator associated pneumonia, length of stay in intensive care and hospital, total duration of mechanical ventilation, and duration of invasive ventilation. It should be noted that most of the trials exclusively enrolled patients with exacerbation of chronic obstructive pulmonary disease; benefits in other types of ventilated patients remain to be firmly proven.
BMJ. 2009 May 21;338:b157
http://www.ncbi.nlm.nih.gov/pubmed/19460803
Ventilator-associated tracheobronchitis
Ventilator associated pneumonia (VAP) is a well recognised complication of ICU care, but colonisation and infection further up the respiratory tract may be a risk factor for VAP that is worth identifying and treating. Ventilator-associated tracheobronchitis (VAT) has similar diagnostic criteria to VAP, but without the radiographic infiltrates.
Ventilator-associated tracheobronchitis: the impact of targeted antibiotic therapy on patient outcomes
Chest. 2009 Feb;135(2):521-8
