Pre-term infants lacking surfactant often require mechanical ventilation, but the consequent barotrauma and volutrauma may contribute to chronic lung disease, or bronchopulmonary dysplasia. Consequently high frequency oscillatory ventilation (HFOV) has been tried, but results from trials are mixed. A new systematic review of 3229 preterm newborns of less than 35 weeks’ gestation in 10 randomised trials fails to show a benefit of HFOV over conventional ventilation.
Elective high-frequency oscillatory versus conventional ventilation in preterm infants: a systematic review and meta-analysis of individual patients’ data
The Lancet, Volume 375, Issue 9731, Pages 2082 – 2091, 12 June 201o
Tag Archives: NLS
Target Oxygen Saturation in Extreme Prems
1316 infants who were born between 24 weeks 0 days and 27 weeks 6 days of gestation were randomised to one of two different target ranges of oxygen saturation: 85 – 89% vs. 91 – 95%. The primary outcome was a composite of severe retinopathy of prematurity (defined as the presence of threshold retinopathy, the need for surgical ophthalmologic intervention, or the use of bevacizumab), death before discharge from the hospital, or both.
All infants were also randomly assigned to continuous positive airway pressure or intubation and surfactant in a 2-by-2 factorial design.
The rates of severe retinopathy or death did not differ significantly between the lower-oxygen-saturation group and the higher-oxygen-saturation group (28.3% and 32.1%, respectively; relative risk with lower oxygen saturation, 0.90; 95% confidence interval [CI], 0.76 to 1.06; P=0.21). Death before discharge occurred more frequently in the lower-oxygen-saturation group (in 19.9% of infants vs. 16.2%; relative risk, 1.27; 95% CI, 1.01 to 1.60; P=0.04), whereas severe retinopathy among survivors occurred less often in this group (8.6% vs. 17.9%; relative risk, 0.52; 95% CI, 0.37 to 0.73; P<0.001). There were no significant differences in the rates of other adverse events.
An editorial notes that the unmasked trial data showed that the distribution of oxygen saturation levels was within or above the target range in the higher-oxygen-saturation group, but in the lower-oxygen-saturation group, it was about 90 to 95% (i.e., above the target range). The difference in oxygen saturation levels between the groups was about 3 percentage points instead of the 6 percentage points that had been planned. Therefore, this study actually compared saturation levels of about 89 to 97% with saturation levels of 91 to 97%; the results should be ascribed to these higher ranges.
Targeting oxygen saturation levels is difficult, and a recommended oxygen saturation range that is effective yet safe remains elusive. A lower oxygen saturation level significantly reduces the incidence of severe retinopathy of prematurity but may increase the rate of death.
Target Ranges of Oxygen Saturation in Extremely Preterm Infants
N Engl J Med. 2010 May 16. [Epub ahead of print]
Early CPAP versus Surfactant in Extreme Prems
In a randomised, multicentre trial of 1316 infants born between 24 weeks 0 days and 27 weeks 6 days of gestation, infants were randomly assigned to intubation and surfactant treatment (within 1 hour after birth) or to CPAP treatment initiated in the delivery room, with subsequent use of a protocol-driven limited ventilation strategy. The primary outcome was death or bronchopulmonary dysplasia as defined by the requirement for supplemental oxygen at 36 weeks.

Infants who received CPAP treatment, as compared with infants who received surfactant treatment, less frequently required intubation or postnatal corticosteroids for bronchopulmonary dysplasia (P<0.001), required fewer days of mechanical ventilation (P=0.03), and were more likely to be alive and free from the need for mechanical ventilation by day 7 (P=0.01). However the rates of the primary outcome did not differ significantly between the CPAP group and the surfactant group (47.8% and 51.0%, respectively; relative risk with CPAP, 0.95; 95% confidence interval [CI], 0.85 to 1.05).
The infants randomised to CPAP could receive limited invasive ventilation if necessary; 83.1% of the infants in the CPAP group were intubated. They did not include infants who were born at a gestational age of less than 24 weeks, since the results of a pilot trial showed that 100% of such infants required intubation in the delivery room.
This study had a 2-by-2 factorial design in which infants were also randomly assigned to one of two target ranges of oxygen saturation.
Early CPAP versus Surfactant in Extremely Preterm Infants
N Engl J Med. 2010 May 16. [Epub ahead of print]
Optimum depth of neonatal chest compressions
A retrospective study of infant chest CT scans using mathematical modelling and a number of assumptions suggests that neonatal CPR according to AAP/AHA guidelines of compressing to one third anteroposterior chest wall diameter should provide a superior ejection fraction to 1/4 depth and should generate less risk for over-compression than 1/2 AP compression depth.
Evaluation of the Neonatal Resuscitation Program’s recommended chest compression depth using computerized tomography imaging
Resuscitation. 2010 May;81(5):544-8
Compare their conclusions with those of the authors of this case series of arterial-line monitored cardiac arrests in infants with a median age of one month
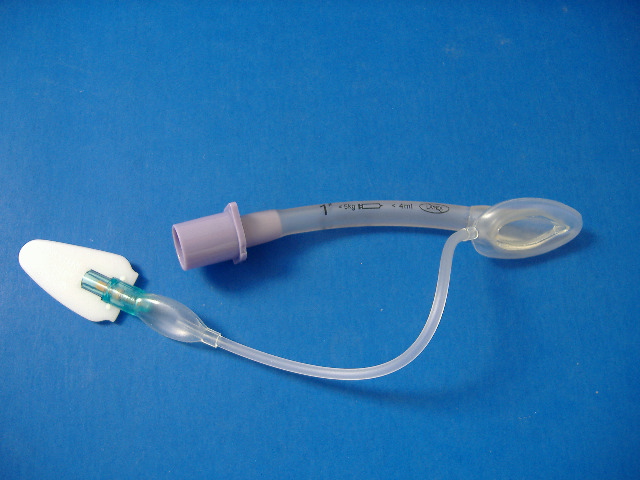
LMA for newborn resuscitation
An observational study of near term infants (34 weeks gestation to 36 weeks and 6 days) born in an Italian centre over a 5 year period showed that nearly 10% of near-term infants needed positive pressure ventilation at birth, confirming that this group of patients is more vulnerable than term infants. Most were able to be managed with either bag-mask ventilation (BMV) or with a size 1 laryngeal mask airway (LMA). Of the 86 infants requiring PPV, 36 (41.8%) were managed by LMA, 34 (39.5%) by BMV and 16 (18.6%) by tracheal intubation. Why not slap a tiny LMA on your neonatal resuscitation cart – it could come in handy!
Delivery room resuscitation of near-term infants: role of the laryngeal mask airway
Resuscitation. 2010 Mar;81(3):327-30
Neonatal prostaglandin E1 and apnoea
The risk of apnoea in neonates requiring prostaglandin E1 infusions for duct-dependent congenital heart disease is well described and often results in the recommendation to intubate prior to transfer. An American study of 202 transported infants on PGE1 shows a higher rate of transport-related complications in those that had been intubated. None of the 73 (36%) unintubated patients required intubation for apneoa during transport. These data are in keeping with a previous Australian study of 300 infants receiving PGE1 in which only 2 of 78 unintubated patients experienced apnoea.
To intubate or not to intubate? Transporting infants on prostaglandin E1
Pediatrics. 2009 Jan;123(1):e25-30