Steroids are useful in asthma and COPD exacerbations, which are lung problems. Pneumonia is a lung infection, so steroids might help there too right? Erm… no.
A double blind randomised controlled trial demonstrated no benefit from steroids (prednisolone) versus placebo in patients with community acquired pneumonia, and late therapaeutic failure (>72 h after admission) was more common in the prednisolone group.
Efficacy of Corticosteroids in Community-acquired Pneumonia: A Randomized Double-Blinded Clinical Trial
Am J Respir Crit Care Med. 2010 May 1;181(9):975-82
Pre-hospital RSI successes
A couple of papers in Prehospital Emergency Care this month contribute to the pre-hospital airway management / rapid sequence intubation (RSI) literature.
Intensive physician oversight of a pre-hospital RSI program increased the prescription of post-intubation morphine and midazolam, and decreased vecuronium use, although did not significantly increase the successful intubation rate in a before-and-after study. There was also an improvement in patient selection for RSI.
Effect of intensive physician oversight on a prehospital rapid-sequence intubation program
Prehosp Emerg Care. 2010 Jul-Sep;14(3):310-6
A prospective study examined intubation success rates and peri-intubation hypoxaemia in critical care transport (CCT) services in North America, whose services are mainly crewed by registered nurses (RNs) and emergency medical technicians–paramedic (EMT-Ps).
There was a mixture of pre-hospital and interhospital work: 51.9% of the 603 patients studied were intubated at the trauma scene, 27% were intubated inside a hospital, and interestingly 21.1% were intubated inside a vehicle (most of which were helicopters).
Neuromuscular blockade was used to facilitate intubation in only 428 patients (71%). Endotracheal intubation (ETI) was successful in 582 patients (96.5% of 603, 95% CI 94.7-97.8%). There was a greater need (p < 0.001) for multiple attempts at ETI when CCT crews performed the procedure in transport (37.3%) as compared with rate of requirement for multiple ETI attempts while in hospital (16.6%) or on scene (19.4%). Logistic regression identified a three-fold increase in the odds of requiring multiple attempts for intratransport ETI as compared with in-hospital ETI (OR 3.0, 95 CI 1.7–5.2, p < 0.001). 21 patients (3.5%) could not be intubated by the CCT crews resulting in a number of different rescue modalities including 3 cricothyroidotomies. At least there were no unrecognised oesophageal intubations. There were low rates of new hypoxaemia but peri-ETI SpO2 was only recorded for 494 patients (82%).
Airway management success and hypoxemia rates in air and ground critical care transport: a prospective multicenter study
Prehosp Emerg Care. 2010 Jul-Sep;14(3):283
Pre-hospital chest escharotomy
Two cases are described in Pre-hospital Emergency Care of severely burned patients who were impossible to adequately ventilate after tracheal intubation until they underwent escharotomy by a pre-hospital physician.
The review that follows reminds us of some intersting escharotomy facts:
- circumferential extremity burns can cause limb ischaemia
- abdominal burns can cause elevated intra-abdominal pressure and ischemic bowel
- neck burns can cause tracheal and jugular venous compression
- chest burns can cause respiratory compromise
- one previous study showed that chest and abdominal escharotomies significantly decreased intra-abdominal pressure, retention of carbon dioxide, and central venous and inferior vena caval pressures while significantly increasing serum oxygen concentration and systolic blood pressure.
- escharotomies may be performed on multiple body parts, including the extremities, the digits, the chest, the abdomen, the neck, and the penis
- neck escharotomy is a relatively simple procedure that involves an incision of the skin eschar longitudinally in the anterior midline from the chin to the sternal notch
- although different ways of doing chest escharotomies have been described, in the two reported cases in this article the procedure only involved longitudinal incisions, with good immediate effect.
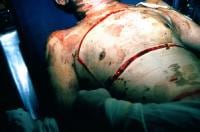
Of note, neither of the physicians concerned had seen or done an escharotomy before. I’m adding this to my list of life-saving surgical interventions that are technically straightforward to perform, cannot always wait for another specialist to do, and happen too rarely to train for in the traditional way (ie being taught on a patient under supervision prior to the first time you do one).
Out-of-hospital chest escharotomy: a case series and procedure review
Prehosp Emerg Care. 2010 Jul-Sep;14(3):349-54
Two tier trauma team
Rather than activating a full trauma team based on traditional criteria, this team devised a two tier approach; if there were no positive anatomical or physiological criteria, a trauma team ‘consult’ approach was adopted, in which the patient was evaluated by emergency department and general surgery doctors only.

Of 1144 trauma activations, 468 (41%) were full trauma and 676 (59%) were consult trauma activations.. Sensitivity of the triage tool for the major trauma outcome (ISS>15, death, or needing critical care or urgent surgery) was 83%, specificity was 68%, undertriage was 3% and overtriage was 27%. There were no deaths in undertriaged patients.
This is an important study that has the potential to improve resource utilisation and even patient experience.
Prospective evaluation of a two-tiered trauma activation protocol in an Australian major trauma referral hospital
Injury. 2010 May;41(5):470-4
Military pre-hospital thoracotomy
Military doctors in Afghanistan reviewed their experience of thoracotomy done within 24 hours of admission to their hospital. The ballistic nature of thoracic penetrating trauma (mainly Afghan civilians without body armour) differs from the typical knife-wound related injury seen in survivors of thoracotomy reported in the pre-hospital literature.
Six of the patients presented in cardiac arrest – four PEA and two asystole. One of the PEA patients survived; this patient had sustained a thoracoabdominal GSW and had arrested 8 minutes from hospital. Following emergency thoracotomy, aortic control, and concomitant massive transfusion, return of spontaneous circulation (ROSC) was achieved and damage control surgery undertaken in both chest and abdomen.
The two patients in asystole had sustained substantial pulmonary and hilar injuries, and ROSC was never achieved. The patients in PEA all had arrested as a consequence of hypovolaemia from solid intra-abdominal visceral haemorrhage. All patients in PEA had ROSC achieved, albeit temporarily.
Following thoracotomy, patients required surgical manoeuvres such as pulmonary hilar clamping, packing and temporary aortic occlusion; hypovolaemia was the leading underlying cause of the cardiac arrest. These factors lead the authors to conclude that although isolated cardiac wounds do feature in war, they are unusual and the injury pattern of casualties in conflict zones are often complex and multifactorial.
Is pre-hospital thoracotomy necessary in the military environment?
Injury. 2010 Jul;41(7):1008-12
New meningococcal guideline
The UK’s National Institute for Health and Clinical Excellence has produced a guideline on the management of bacterial meningitis and meningococcal septicaemia in children.
The guidelines cover when to treat a petechial rash, when to give steroids, when to do an LP (and what to test), how much fluid to give, and a number of other areas that otherwise can cause confusion.
The management of bacterial meningitis and meningococcal septicaemia in children and young people younger than 16 years in primary and secondary care
NICE guidance
Infant CPR: two thumbs even when alone
Infant CPR guidelines recommend two-finger chest compressions with a lone rescuer and two-thumb with two rescuers. Two-thumb provides better chest compression but is perceived to be associated with increased ventilation hands-off time. A manikin study revealed more effective compressions with the two-thumb technique with only four fewer compressions per minute compared with two-fingers.

Two-thumb technique is superior to two-finger technique during lone rescuer infant manikin CPR
Resuscitation. 2010 Jun;81(6):712-7
Valsalva technique in SVT
Investigators at the Royal North Shore Hospital in Sydney (it’s good there) did a literature review to determine the best ‘gold standard’ way of performing a Valsalva manoeuvre for SVT, and assessed success rates before and after its introduction into the ED.
The technique required the patient to lie supine on the bed in a Trendelenberg position, and forcefully expire into a section of suction tubing and pressure gauge for at least 15 seconds and at a pressure of at least 40 mm Hg. The theory behind increased success in a supine position lies in augmenting the patients’ vagal tone and attenuating the sympathetic tone in addition to increased venous return during phase IV of Valsalva. The ‘standardised’ technique improved the rate of successful termination of SVT from 5.3% to 31.7%
Impact of a modified Valsalva manoeuvre in the termination of paroxysmal supraventricular tachycardia
Emerg Med J. 2010 Apr;27(4):287-91
Surviving avalanche burial

Avalanche burial has a high mortality and yet in some cases there have been some amazing saves despite prolonged cardiac arrest. An international working group undertook a systematic review to examine 4 critical prognostic factors for burial victims in cardiac arrest. You have a better chance of surviving a prolonged burial if you have a patent airway and a pocket of air (even a very small one), are hypothermic, and preferably not hyperkalaemic.
Prognostic factors in avalanche resuscitation: A systematic review
Resuscitation. 2010 Jun;81(6):645-52
Pre-hospital RSI
Physicians from HEMS London document their experience of 400 pre-hospital rapid sequence induction / intubations. Their data are consistent with the experience of other similar services and with the emergency airway management literature in general:
- Failure to intubate is rare
- Removing cricoid pressure often improves the view
- A BURP manoeuvre can improve the view and facilitate intubation, but bimanual laryngoscopy / external laryngeal manipulation is better
- Having an SOP optimises first-pass success rate
Cricoid pressure and laryngeal manipulation in 402 pre-hospital emergency anaesthetics: Essential safety measure or a hindrance to rapid safe intubation?
Resuscitation 2010(81):810–816
