Even though we might not know it’s called that, many of us are familiar with the Baux score, defined as the sum of age in years and percent body burn, to predict percent mortality after severe burns. This is however a little out of date due to advances in burn care, and does not take into account inhalational injury.
The Baux score was modified using data on 39,888 burned patients using a logistic regression model that showed that age and percent burn contribute almost equally to mortality and that the presence of inhalation injury added the equivalent of 17 years (or 17% burn). These observations suggested a revised Baux Score:
Per Cent Mortality = Age + Percent Burn + [17 x (Inhalation Injury, 1= yes, = no)]
Simplified Estimates of the Probability of Death After Burn Injuries: Extending and Updating the Baux Score
J Trauma. 2010 Mar;68(3):690-7
Monthly Archives: March 2010
College of Paramedics stands its ground
Articles in this month’s EMJ demonstrate an interesting conflict within UK pre-hospital care. The Joint Royal Colleges Ambulance Liaison Committee Airway Working Group, heavily represented by anaesthetists, recommend the removal of tracheal intubation from UK paramedic practice. The College of Paramedics reject this recommendation, providing a robust critique of the paper and calling for better evidence before changing current practice. A fascinating read.
A critical reassessment of ambulance service airway management in prehospital care: Joint Royal Colleges Ambulance Liaison Committee Airway Working Group, June 2008
Emerg Med J 2010;27:226-233
Full Text
The College of Paramedics (British Paramedic Association) position paper regarding the Joint Royal Colleges Ambulance Liaison Committee recommendations on paramedic intubation
Emerg Med J 2010;27:167-170
Full Text
Guidelines on penetrating abdominal trauma
The Eastern Association for the Surgery of Trauma has published guidelines on the nonoperative management of penetrating abdominal trauma.
RECOMMENDATIONS
- Patients who are hemodynamically unstable or who have diffuse abdominal tenderness should be taken emergently for laparotomy (level 1).
- Patients who are hemodynamically stable with an unreliable clinical examination (i.e., brain injury, spinal cord injury, intoxication, or need for sedation or anesthesia) should have further diagnostic investigation performed for intraperitoneal injury or undergo exploratory laparotomy (level 1).
- A routine laparotomy is not indicated in hemodynamically stable patients with abdominal stab wounds (SWs) without signs of peritonitis or diffuse abdominal tenderness (away from the wounding site) in centers with surgical expertise (level 2).
- A routine laparotomy is not indicated in hemodynamically stable patients with abdominal gunshot wounds (GSWs) if the wounds are tangential and there are no peritoneal signs (level 2).

- Serial physical examination is reliable in detecting significant injuries after penetrating trauma to the abdomen, if performed by experienced clinicians and preferably by the same team (level 2).
- In patients selected for initial nonoperative management, abdominopelvic CT should be strongly considered as a diagnostic tool to facilitate initial management decisions (level 2).
- Patients with penetrating injury isolated to the right upper quadrant of the abdomen may be managed without laparotomy in the presence of stable vital signs, reliable examination, and minimal to no abdominal tenderness (level 3).
- The majority of patients with penetrating abdominal trauma managed nonoperatively may be discharged after 24 hours of observation in the presence of a reliable abdominal examination and minimal to no abdominal tenderness (level 3).
- Diagnostic laparoscopy may be considered as a tool to evaluate diaphragmatic lacerations and peritoneal penetration (level 2).
Practice Management Guidelines for Selective Nonoperative Management of Penetrating Abdominal Trauma
J Trauma. 2010 Mar;68(3):721-733
WHO Guidelines for Pandemic Influenza A(H1N1) 2009
The World Health Organisation has published updated guidelines on drug treatment of Influenza A(H1N1)2009 and other influenza viruses. Their recommendations are summarised in this table:

Full text of the guidelines is available here
WHO Guidelines for Pharmacological Management of Pandemic Influenza A(H1N1) 2009 and other Influenza Viruses
WHO website
CT cervical spine in obtunded trauma patients
Prolonged collar use and spinal immobilisation in ICU patients can contribute to pressure sores, increased intracranial pressure, venous obstruction, difficulties with airway management, difficulties with central venous access, respiratory complications, and DVT, so a reliable investigation to rule out unstable cervical spine injury is required. Several studies demonstrate the high sensitivity of CT, and now a prospective study from Canada attempts to lend further support to this.
Comparing against their chosen gold standard of dynamic radiography, ie. flexion/extension views (F/E) in 402 patients who received both tests, there was one case of injury detected by F/E but not by CT, leading to quoted sensitivity of 99.75%. However this negative CT turned out to be a reporting error – the scan, which the authors include in their article, was clearly abnormal.
One weakness of this study is that they excluded patients who died on ICU. More worrying are the stats quoted. The authors stat ‘four hundred one patients (99.75%) had normal CT and F-E images facilitating clinical clearance of their C-spine and discontinuation of spinal precautions‘. So in other words, there was only one patient in their series of 402 with an injury (according to the gold standard), and this was missed. The sensitivity is therefore zero percent, not 99.75%. What seems to be a further error is the reporting in a table of 401 patients who had ‘Positive CT and Negative F-E’, which if true, would give a specificty of zero too!
This paper covers an important topic for intensivists but it seems to me to be too flawed to add meaningfully to the existing evidence that necks can be ‘cleared’ by CT in patients without signs of cervical spine injury, in whom it has been said that the risks of prolonged collar use and immobilisation may outweigh the risks of missed cervical injury.
Cervical spine clearance in obtunded blunt trauma patients: a prospective study
J Trauma. 2010 Mar;68(3):576-82
Echo best test for acute LVF in ED
Three diagnostic tests for acute left ventricular heart failure in dyspnoeic patients were compared, with the gold standard being the diagnosis by three independent reviewers (two cardiologists and one respiratory physician) who were blinded to the results of the tests being examined. The tests in question were NT-proBNP, the Boston criteria, and limited echo performed by emergency physicians.
The primary goal of the echo study was the detection of the following echocardiographic variables, expressed as present or absent: reduced LV ejection fraction (LV ejection fraction <50% on subjective visual estimation of the change in LV size between diastole and systole) and the ‘‘restrictive’’ pattern on pulsed Doppler analysis of mitral inflow (using the apical view).
According to the authors, pulsed Doppler analysis of mitral inflow can be described by three patterns: 1) an ‘‘impaired relaxation’’ pattern, suggesting no increase in LV filling pressures; 2) a ‘‘normal’’ or ‘‘normalized’’ pattern; and 3) a restrictive pattern, suggesting an increase in LV filling pressures.

Trained emergency physicians were able to perform EDecho in a median of 4 minutes, obtaining Doppler data in an average of 80% of patients presenting for acute dyspnea. Considering the 125 patients with both EDecho variables available, reduced LV ejection fraction was less accurate than the restrictive mitral pattern for the diagnosis of aLVHF. The restrictive pattern was more sensitive (82%) and specific (90%) than reduced LV ejection fraction and more specific than the Boston criteria and NT-proBNP for the diagnosis of aLVHF. The accuracy of the restrictive pattern in the overall population was 75%, compared with accuracy of 49% for both NT-proBNP and Boston criteria.
Diagnostic accuracy of emergency Doppler echocardiography for identification of acute left ventricular heart failure in patients with acute dyspnea: comparison with Boston criteria and N-terminal prohormone brain natriuretic peptide.
Acad Emerg Med. 2010 Jan;17(1):18-26
Intubation harder on the floor or in an ambulance
An abstract from the The National Association of EMS Physicians® 2010 Scientific Assembly published in a Supplement of Prehospital Emergency Care describes a study comparing cadaveric intubation success rates by paramedics in different positions: on the floor, on an elevated stretcher, and in a simulated ambulance. Despite less experience intubating on an elevated stretcher, the participants had increased first-attempt success in the elevated stretcher position compared with the back of the ambulance and the floor (although in the latter case this lacked statistical significance). Position is everything! In our HEMS service we prefer a lowered stretcher to either on the ground or in the ambulance – it would be nice to see this position studied one day too.

Pre-hospital intubation: patient position does matter
Prehospital Emergency Care 2010;14(Suppl 1):9
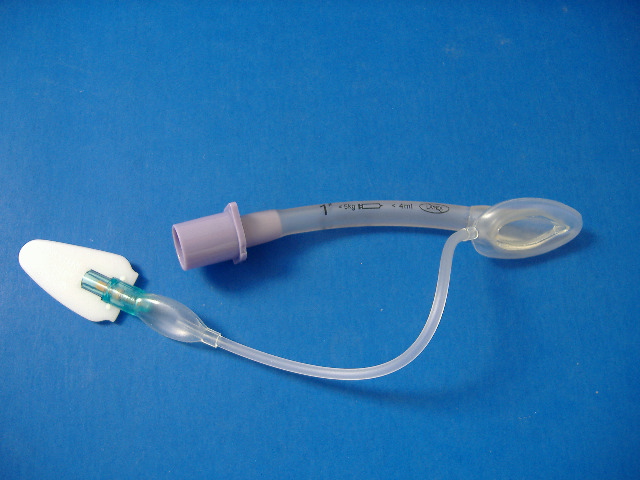
LMA for newborn resuscitation
An observational study of near term infants (34 weeks gestation to 36 weeks and 6 days) born in an Italian centre over a 5 year period showed that nearly 10% of near-term infants needed positive pressure ventilation at birth, confirming that this group of patients is more vulnerable than term infants. Most were able to be managed with either bag-mask ventilation (BMV) or with a size 1 laryngeal mask airway (LMA). Of the 86 infants requiring PPV, 36 (41.8%) were managed by LMA, 34 (39.5%) by BMV and 16 (18.6%) by tracheal intubation. Why not slap a tiny LMA on your neonatal resuscitation cart – it could come in handy!
Delivery room resuscitation of near-term infants: role of the laryngeal mask airway
Resuscitation. 2010 Mar;81(3):327-30
Do all comatose patients need intubation?
In non-trauma patients, do you base your decision to intubate patients with decreased conscious level on the GCS? These guys in Scotland describe a series of poisoned patients with GCS range 3-14 managed on an ED observation unit without tracheal intubation, with no demonstrated cases of aspiration. They say: ‘This study suggests that it can be safe to observe poisoned patients with decreased consciousness, even if they have a GCS of 8 or less, in the ED‘. Small numbers, but gets you thinking. This subject would make a great randomised controlled trial.
Decreased Glasgow Coma Scale score does not mandate endotracheal intubation in the emergency department
J Emerg Med. 2009 Nov;37(4):451-5
Is defibrillation an electric threat for bystanders?
No rescuer or bystander has ever been seriously harmed by receiving an inadvertent shock while in direct or indirect contact with a patient during defibrillation. New evidence suggests that it might even be electrically safe for the rescuer to continue chest compressions during defibrillation if self-adhesive defibrillation electrodes are used and examination gloves are worn. This paper reviews the existing evidence, but warns more definite data are needed to make absolutely sure that there is no risk before defibrillation safety recommendations are changed.

Is external defibrillation an electric threat for bystanders?
Resuscitation. 2009 Apr;80(4):395-401